High Testosterone and Libido in Men? Understanding the Link, Impact, and When to Seek Help
Testosterone is a primary hormonal driver of male libido by activating key brain regions, but sexual desire is a complex interplay of biology, psychology, and lifestyle. Low testosterone can reduce libido, but is not the sole factor.
Testosterone’s Role: A Key Driver of Libido, Not the Whole Story
Testosterone’s role is that of a key biological driver for libido, but it does not represent the entirety of a man’s sexual desire. It’s helpful to think of testosterone as the high-octane fuel for the engine of desire.
While essential for the engine to run powerfully, the experience of driving is also affected by the driver (your psychological state) and the road conditions (your lifestyle and relationship). Even with a full tank of fuel, a stressed driver on a bumpy road may have no interest in going for a ride.
Libido as the *desire* for sex; testosterone as a primary biological *driver* of that desire
Libido is medically defined as the conscious desire for sex, whereas testosterone is the primary biological hormone that helps drive and sustain that desire. Libido is the psychological and emotional state of “wanting,” while testosterone acts as a neurochemical catalyst, stimulating the parts of the brain responsible for arousal and motivation.
This creates a simple but crucial chain of events: Testosterone activates neural pathways, which in turn increases the likelihood of experiencing sexual desire. It’s important not to use these terms interchangeably, as this distinction is key to understanding your sexual health. Libido is about desire, not necessarily performance or erectile function.
How testosterone levels fluctuate naturally and their effect on desire
Testosterone levels in men fluctuate naturally throughout the day, across the week, and over a lifetime, which can cause subtle, temporary changes in sexual desire. Most men experience a diurnal rhythm, with testosterone levels peaking in the morning and gradually decreasing throughout the day. Levels also tend to decline slowly with age, typically by about 1% per year after age 30-40.[1]
These minor, normal fluctuations can lead to everyday variations in libido. This is very different from the significant, persistent drop in desire that might signal a clinical issue. The age-related decline is a gradual process, and many older men maintain healthy and satisfying libidos.
Why high testosterone doesn’t always guarantee high libido, and vice versa
High testosterone does not always guarantee a high libido because sexual desire is also heavily influenced by psychological, relational, and lifestyle factors. This is the core misconception many people have.
Even with optimal hormonal “fuel,” a person experiencing high stress, anxiety, depression, or conflict in their relationship may have little to no desire to “drive.” The brain’s emotional and stress-response centers can effectively override the biological signals from testosterone. Conversely, a man with lower-normal testosterone can have a vibrant libido if psychological, health, and relationship factors are positive and supportive.[2]
How Does Testosterone Activate Male Sexual Desire?
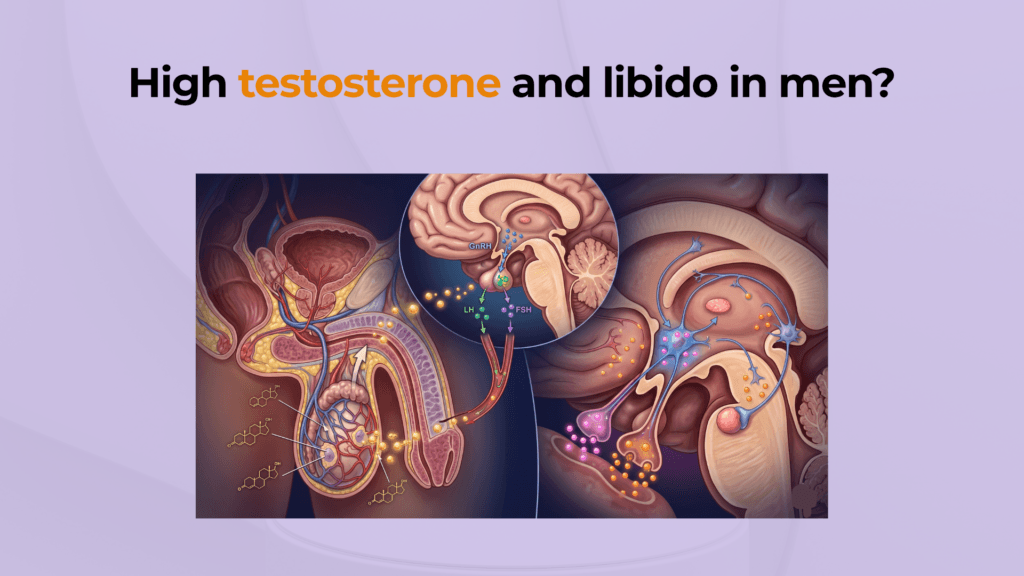
Testosterone activates male sexual desire primarily by binding to androgen receptors in key brain regions, such as the hypothalamus and amygdala, which regulate arousal and motivation. This is not a vague influence; it’s a specific biological process where the hormone travels through the bloodstream, enters the brain, and “switches on” the neural circuits that generate sexual thoughts and interest in response to stimuli.
The impact of testosterone on brain regions associated with sexual arousal and motivation
The primary impact of testosterone on the brain involves stimulating the medial preoptic area (MPOA) of the hypothalamus, which is a critical control center for male sexual behavior.[3] Think of the MPOA as the brain’s accelerator for sexual interest.
Testosterone makes this area, along with the amygdala (involved in emotional processing), more reactive to sexual cues—whether visual, mental, or physical. This increased sensitivity is what translates a hormonal signal into a conscious feeling of desire.
Testosterone’s influence on libido through androgen receptors
Testosterone’s influence on libido is mediated through androgen receptors, which act as docking stations on cells in the brain and body that, once activated by testosterone, trigger a cellular response related to sexual function. This is often called the “lock and key” mechanism: testosterone is the key, and the androgen receptor is the lock.
When the key fits into the lock, it opens the door to a cascade of neurochemical events that promote libido. Without a sufficient number of functioning receptors, even high levels of testosterone may have a diminished effect.
The link between free testosterone and its availability to tissues
The critical link to libido is primarily with free testosterone, which is the unbound, biologically active portion of the hormone that is available to enter tissues and activate androgen receptors. The vast majority of testosterone in the bloodstream is bound to proteins, mainly Sex Hormone-Binding Globulin (SHBG), rendering it inactive.
Only a small fraction, typically around 1-2%, is “free.”[4] This is why a standard blood test for *total* testosterone might not tell the whole story; a person could have normal total levels but low free testosterone, which could contribute to lower libido.
Beyond Testosterone: Other Critical Factors Affecting Male Libido
Beyond testosterone, other critical factors affecting male libido include psychological health, lifestyle habits, other hormones, and underlying medical conditions. A comprehensive understanding requires looking at the whole person, not just a single hormone level. This is where the simple “fuel in the tank” analogy breaks down, and we must consider the entire system.
Psychological factors: Stress, anxiety, depression, and relationship issues
Mental and emotional states can powerfully override biological drivers of libido. Chronic stress elevates cortisol, a hormone that can suppress testosterone production. Anxiety and depression can consume mental bandwidth, leaving little room for sexual thoughts and feelings.
Furthermore, unresolved conflict, poor communication, or a lack of emotional intimacy in a relationship can be one of the strongest libido inhibitors.[2]
Lifestyle factors: Diet, exercise, sleep, and substance use
Healthy lifestyle habits are foundational for a healthy libido. Poor sleep is particularly detrimental, as it disrupts the body’s entire hormonal cascade. A sedentary lifestyle and a diet high in processed foods can contribute to obesity and poor metabolic health, both of which negatively impact testosterone.
Excessive alcohol use can suppress the central nervous system and lower desire, while other substances can have even more profound effects.[5]
Other hormonal influences: Prolactin, thyroid hormones, and cortisol
Testosterone doesn’t operate in a vacuum. High levels of the hormone prolactin, for instance, are known to suppress libido. An underactive or overactive thyroid can throw off the body’s metabolism and energy levels, indirectly affecting sexual desire. As mentioned, high levels of the stress hormone cortisol can also interfere with testosterone’s effects.[6]
Medical conditions and medications impacting libido
Certain medical conditions like diabetes and heart disease, along with medications such as antidepressants and blood pressure drugs, can significantly impact libido independent of testosterone levels. Conditions that affect blood flow or nerve function can diminish arousal.
Many common medications, particularly SSRIs (a class of antidepressants) and beta-blockers, are known to have sexual side effects, including reduced desire.[7]
| Factor Category | Key Influencers | How It Impacts Libido |
|---|---|---|
| Testosterone | Free Testosterone Levels | Directly fuels the biological drive for sex by activating brain regions for arousal. |
| Psychological | Stress, Anxiety, Depression | Occupies mental bandwidth, increases cortisol, and reduces the capacity for sexual thoughts and intimacy. |
| Lifestyle | Poor Sleep, Diet, Lack of Exercise | Depletes energy, disrupts hormone regulation, and negatively impacts mood and self-esteem. |
| Relational | Conflict, Lack of Intimacy | Emotional distance and unresolved issues can override biological desire. |
| Other Hormones | High Prolactin, Thyroid Issues | Can directly suppress libido and interfere with testosterone’s effects. |
| Medications | SSRIs, Beta-blockers | Can have side effects that directly lower sexual desire or arousal. |
How to Assess Your Own Libido and Potential Testosterone Link
Before jumping to conclusions about your hormone levels, it’s productive to engage in some structured self-reflection. This can help you identify patterns and provide a healthcare professional with high-quality information, leading to a more accurate and efficient diagnosis.
What to note before consulting a healthcare provider
Before consulting a healthcare provider, you should note the duration and severity of your low libido, any accompanying symptoms, and a summary of your lifestyle and stress levels. Organizing your thoughts beforehand makes for a much more productive doctor’s visit. Use the following checklist to prepare.
-
✓Libido Pattern: Has my desire decreased gradually or suddenly? How long has this been an issue?
-
✓Symptom Tracking: Am I experiencing other symptoms like fatigue, low mood, irritability, or reduced muscle mass?
-
✓Erectile Function: Is my ability to get or maintain an erection also affected, or is it only a lack of desire?
-
✓Lifestyle Audit: How has my sleep, diet, exercise, and alcohol/substance use been recently?
-
✓Mental Health: Am I experiencing high levels of stress, anxiety, or symptoms of depression?
-
✓Relationship Context: Are there any unresolved issues or emotional distance in my relationship?
When Does Low Libido in Men Warrant Medical Evaluation?
While occasional dips in libido are normal, a persistent lack of desire that causes personal distress or affects your relationship warrants a conversation with a healthcare provider. According to clinical guidelines, evaluation for low testosterone (hypogonadism) is recommended when a man consistently displays symptoms—like low libido—in addition to having demonstrably low testosterone levels in the blood.[8] The key is the combination of persistent symptoms and clinical findings.
What to expect during a medical evaluation: Blood tests, discussion of symptoms, and treatment options
During a medical evaluation for low libido, you can expect a detailed discussion of your symptoms, a physical exam, and blood tests to check total and free testosterone, among other health markers. The doctor will use the information you prepared (from the checklist above) to build a complete picture.
They will likely order a blood test, ideally in the morning when testosterone is highest. Based on the results and your overall health, they will discuss potential causes and a range of treatment options, which may include lifestyle changes, therapy, or, if indicated, testosterone replacement therapy.
| Symptom / Situation | Recommended Action | Rationale |
|---|---|---|
| Curiosity or minor fluctuation | Monitor & Lifestyle Audit | Normal variations occur; assess lifestyle factors first. |
| Persistent low desire (months) impacting well-being | Schedule a Doctor’s Appointment | A chronic change warrants a baseline check-up and discussion. |
| Low libido PLUS other symptoms (fatigue, depression, erectile dysfunction) | Schedule a Doctor’s Appointment | A cluster of symptoms suggests a potential underlying systemic or hormonal issue. |
| Sudden and complete loss of libido | Schedule an Urgent Doctor’s Appointment | A rapid, severe change could indicate a more acute medical issue. |
The Holistic View: Balancing Testosterone, Health, and Desire
Ultimately, male libido is not a simple equation of “more testosterone equals more desire.” It is a multifactorial experience deeply intertwined with your mental, physical, and relational health.
While testosterone provides the crucial biological foundation, a healthy and fulfilling sex drive is the product of overall well-being. A holistic approach—one that addresses stress, prioritizes sleep, encourages a healthy lifestyle, and fosters emotional connection—is the most effective path to balancing hormones, health, and desire for the long term.